How Many Units of Botox For TMJ?
- David Chen, DDS
- Apr 16, 2024
- 3 min read
Updated: Apr 24, 2024
On average, 50-100 units of Botox is recommended for effective TMJ treatment with 50 units as the starting dose and 100 units reserved for severe TMD. The botox may be injected into just the masseter muscle or in combination with the temporalis muscle.
TMJ Botox Overview:
Minimum starting dose
If it is your first time getting botox for your TMJ, you will most likely receive a starting dose of 50 units, 25 units on the left side and 25 units on the right side. The amount can be split between the masseter and temporalis or given solely to the masseter muscle.

Why start with 50 units: We start with a lower dose to see how your body responds to the botox. For some people, this may be more than adequate to significantly relieve their TMJ pain and they may not need any more. Giving too much at once can be detrimental.
How we do it: Our dentists prefer to start with 50 units split evenly between the left masseter and right masseter muscle. That means you'll get 25 units injected into the left and 25 units into the right side.
The minimum dose will also be the treatment that costs the least.
Can I get less than 50 units of botox for TMJ?
It is possible to receive less than 50 units of botox for temporomandibular joint treatment but it may not be sufficient to freeze the muscle. The masseter muscle is fairly large and very strong so it requires a sizable dose to reduce its activity.
Another important point is that the smallest vial size that botox comes in is 50 units. It would be wasteful to discard the rest and not use it.
Maximum dose
Typically, you don't want to have more than 100 units of botox injected for TMD treatment because too much can completely inactivate the TMJ muscles.
Consequences of too much botox injected into TMJ muscles:
Unable to chew and eat your food properly.
Speech issues such as poor enunciation.
Difficulty opening and closing mouth.
The TMJ muscles may be contributing to your jaw pain but at the same time, they also control your ability to eat and also your speech. Having too much injected will make daily activities in your life much more difficult.
How to tell if you've had too much botox for your TMJ
A tell tale sign of having received too much botox is if you need a fork and knife to eat all of your food. That means if you have to cut up all of your food with a knife in order to eat it... perhaps you should consider a smaller dose of botox at your next visit.
Muscles injected for TMJ botox
The two most commonly injected muscles for TMJ botox are the masseter and temporalis. The TMJ muscles actually consist of four muscles but the other two aren't commonly injected for this treatment.
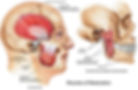
TMJ muscles:
Masseter
Temporalis
Medial pterygoid
Lateral pterygoid
Why the pterygoids aren't injected: Both the medial and lateral pterygoids aren't as easily accessible for botox injections. Customarily, most clinicians will not inject those two muscles. However, it doesn't mean that it can't be done but most of the time, just freezing the masseter and temporalis provides sufficient jaw pain relief.
Overall you can expect to see effects within 1-2 weeks.
Verdict
Botox for TMJ requires 50-100 units for effective TMD treatment and consequently a reduction of jaw pain and pain relief. If you're suffering from TMJ related jaw pain, our dentists can help you because we offer TMJ botox in Long Island City.
